In the rapidly evolving modern world, technological advancements are allowing for more effective research and treatment of diseases, disorders, and injuries sustained by humans. One of the foremost areas of current research in the biomechanics field is that of its role in treatment and rehabilitation of neurological disorders such as amyotrophic lateral sclerosis (ALS) and multiple sclerosis (MS). According to the United Nations, as many as 1 billion people in the world live with neurological disorders. This post will focus mainly on how biomechanics can aid in the treatment and rehabilitation of ALS and MS.
Continue reading “Biomechanics: a Key Factor in Rehabilitation of Neurological Diseases”Month: March 2019
Exciting Advance in ACL Repair
Anterior Cruciate Ligament (ACL) injuries are among the most common in sports, with nearly 100,000 tears annually. Additionally, the rate of pediatric tears has been increasing at a rate of 2.3% each year for the past 20 years. The high incidence of this injury is in part due to the structure of the knee complex, where the ACL is located. The ACL helps connect the two longest bones in the body and is responsible for rotation and transferring body weight to the ankle. Specifically, the primary functions of the ACL are to prevent the tibia from sliding too far in front of the femur and to provide rotational stability to the joint. This rotational motion, combined with a lack of muscle support at the knee, is why so many athletes tear their ACL. A recent paper looked into how a team of doctors led by Dr. Martha Murray at Boston Children’s Hospital have come up with a promising new approach to repairing the injured ligament.
Continue reading “Exciting Advance in ACL Repair”Scleroderma and Raynaud’s Phenomenon: Cold Weather’s Influence on Skin
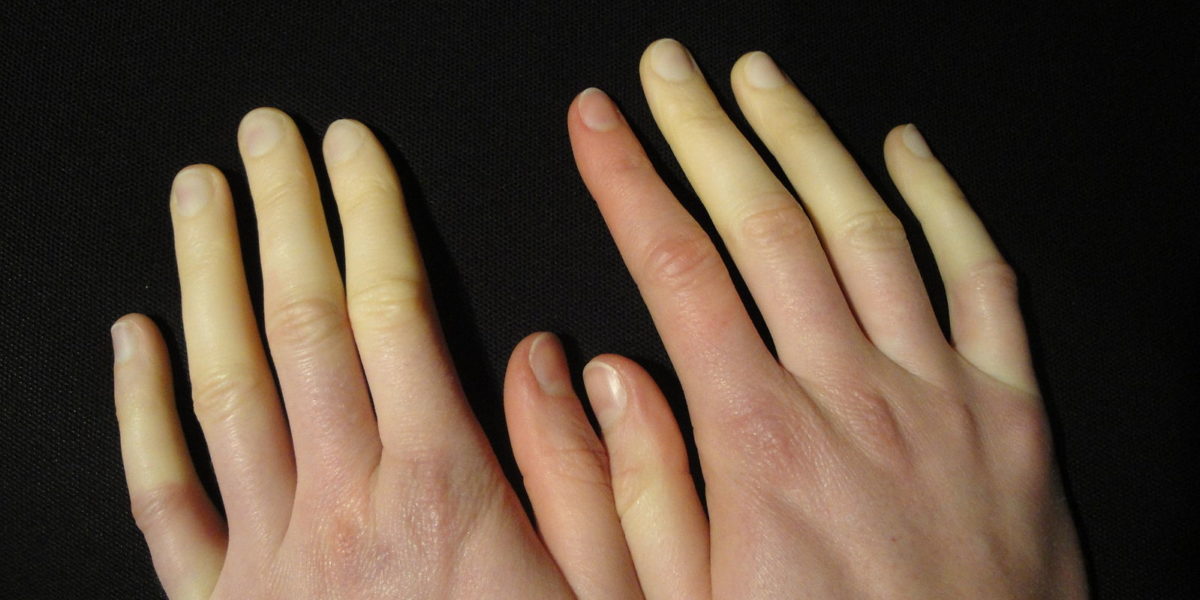
Anyone who is familiar with winters that are mainly at temperatures in single digit range knows how crucial gloves are to surviving the tough, frigid weather. If one was to go outside without them, their hands become extremely pale (or sometimes almost blue) and, once back inside, take a bit of time to get back to normal. It’s a tough life, I know, but people with a scleroderma have an even harder time surviving the winter. What is scleroderma, you ask? Scleroderma is an autoimmune disease that causes skin and internal organs to thicken, and if that wasn’t tough enough, a good chunk of people with it also experience secondary Raynaud’s phenomenon, which is an exaggerated vasoconstriction of arterioles in response to cold weather and causes a drop in blood flow. The main, visible outcome from this disease is how the skin whitens and swells. Problems must ensue from the combination of thick skin and lack of blood flow to the extremities, right?
Continue reading “Scleroderma and Raynaud’s Phenomenon: Cold Weather’s Influence on Skin”Fish in Flight: The Science Behind Great White Breach Attacks on Cape Fur Seals
If you’ve ever turned on Discovery channel during Shark Week, then you’ve probably seen the iconic footage of a 2.5-ton great white shark leaping out of the water to catch its next meal. If you’re weird like me and you’ve ever tried to mimic one of these epic breaches in a backyard pool, then you realize just how difficult it is to generate enough momentum to jump even partway out of the water and therefore have a real appreciation for what it takes to pull off this incredible feat.
Continue reading “Fish in Flight: The Science Behind Great White Breach Attacks on Cape Fur Seals”The Unfair Advantage: Prosthetics and Their Role in the Olympics
In 2012, the “Blade Runner” Oscar Pistorius became the first double amputee to compete in the Olympics. Ever since this historic occasion, the issue of whether prosthetics should be allowed in athletics has been a topic of controversy in the media. Do prosthetics give amputees an advantage over able-bodied athletes? Are athletes with prosthetics capable of running faster and performing better than able-bodied athletes?
Continue reading “The Unfair Advantage: Prosthetics and Their Role in the Olympics”Artificial Turf: Game Changer or Game Ender?
Artificial turf fields were first introduced in the late 1960s and have grown tremendously in popularity since. Today, artificial turf fields can be found at all levels of sport, from youth league to professional, and across many different sporting disciplines. A major reason they are so popular is because they offer a consistent, low-maintenance, year-round green playing field in all weather conditions and climates. However, despite the benefits they provide, artificial turf fields are not without controversy. Even though artificial turf mimics grass in appearance, its properties are much different.
Continue reading “Artificial Turf: Game Changer or Game Ender?”Muscle Loss Due to Aging
It is a well-known fact that as we get old, our bodies (sadly) deteriorate, leaving us unable to perform certain physical functions as easily as we could have when we were younger. In this article, the authors describe a study done to analyze muscle loss due to aging, primarily by examining two different age groups of humans. By conducting measurements on people over and under the age of 40 years, results show a clear difference in muscle mass and strength between the two.
Continue reading “Muscle Loss Due to Aging”High Heels: How They Can Affect You Even After You Take Them Off
Anyone who has worn high heels, or has even simply seen a person in high heels, knows that the foot is definitely not in its usual position in that kind of shoe – walking is more difficult and forget about even trying to run in high heels. Researchers from Manchester Metropolitan University and the University of Vienna wanted to investigate if frequent, long term use of high heels caused lasting changes in the calf, in addition to the normal discomfort experienced by high heel wearers.
Continue reading “High Heels: How They Can Affect You Even After You Take Them Off”Walk [Under] Water: The Benefits of Underwater Running
Just because you can’t walk on water doesn’t mean you shouldn’t run under it!
Aqua-jogging. Hydro-running. Water-treadmills. Have you ever heard some combination of these terms and wondered what the hype is?
Continue reading “Walk [Under] Water: The Benefits of Underwater Running”Gainz for Dayz: Conventional vs Sumo Deadlift
What’s the best way to pick stuff up and put it back down?
Continue reading “Gainz for Dayz: Conventional vs Sumo Deadlift”






![Walk [Under] Water: The Benefits of Underwater Running](https://sites.nd.edu/biomechanics-in-the-wild/files/2019/03/hydrotrack-e1680741443448-1200x600.jpg)
