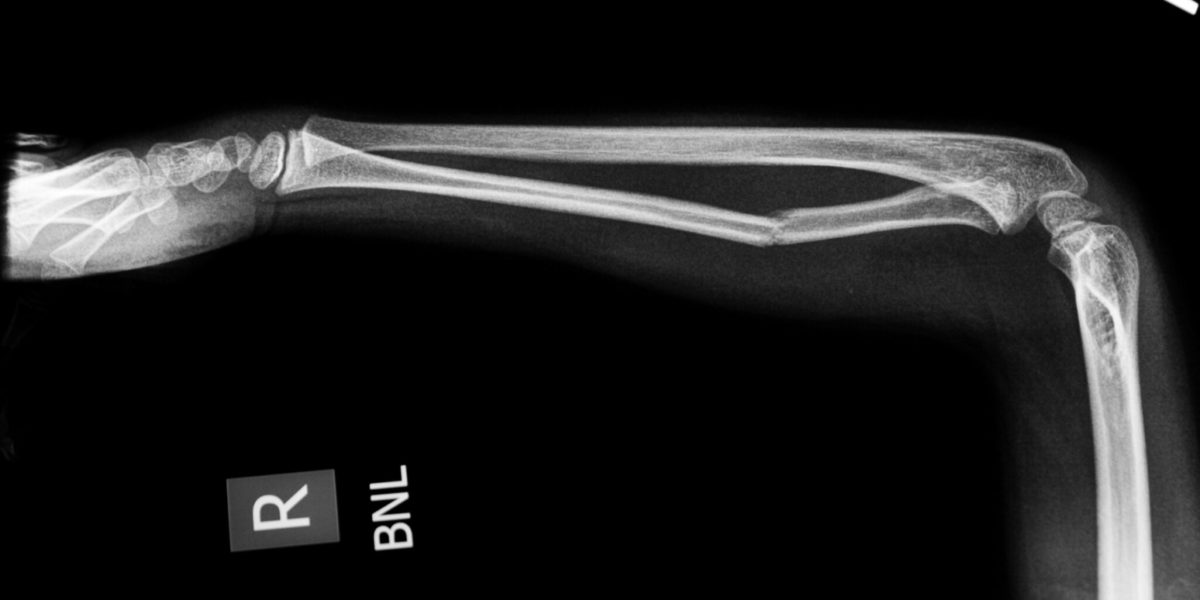
Since World War 2, The use of antipersonnel mines (APMs) have been a key factor in a nation’s military success. The most recent iteration of the APM is the improvised explosive device (IED) often seen in the Global War on Terror (GWOT), utilized by terrorist and guerrilla groups that do not have the manufacturing capabilities of an established military. IEDs have been proven to cause greater damage to their victims than conventional APMs, and the often resulting amputations call for a much more complicated rehabilitation process for service members.
Continue reading “IEDs in the Global War on Terror: A Long Road to Recovery”Tag: other injury
They need some milk! The Link between Cycling and Osteoporosis
Athletes often are pestered about the importance of cross training by coaches and trainers alike. Football players work on flexibility through ballet. Runners, who primarily train in forward movements, practice calisthenics to build up their lateral strength. Similarly, cyclists are encouraged to participate in some contact-related activity. These are all good reasons for why athletes should cross-train, but will something actually happen if they refuse to cross-train? It’s crossed every athlete’s mind, from professionals to enthusiasts: “What’s the worst that could happen?”.
Continue reading “They need some milk! The Link between Cycling and Osteoporosis”Do Shoes Alter the Form and Function of Your Feet?
Have you ever worn a favorite pair of shoes much longer than you should’ve, only to experience an injury as a result? What if I told you that a large portion of modern footwear might increase your injury risk, even when brand new?
Continue reading “Do Shoes Alter the Form and Function of Your Feet?”Do your Foot Arches make you more or less likely to be injured?
Have you ever wondered how your arch type may affect your everyday life especially in physical activities such as running or playing sports? Well it turns out that without taking precautions, a higher arch or a flat foot may cause you to more likely be injured! People have all different types of arches, and each foot can be affected differently based on the type of arch.
Continue reading “Do your Foot Arches make you more or less likely to be injured?”Have you ever wondered how your arch type may affect your everyday life especially in physical activities such as running or playing sports? Well it turns out that without taking precautions, a higher arch or a flat foot may cause you to more likely be injured! People have all different types of arches, and each foot can be affected differently based on the type of arch.
Continue reading “Do your Foot Arches make you more or less likely to be injured?”Ditching the shoes: Minimalist trend or natural advantage?
The discussion of returning to minimalist ways, namely walking or running barefoot, is a question that rises in many circles, from new parents to elite runners.
Continue reading “Ditching the shoes: Minimalist trend or natural advantage?”Top Gun Trauma: the Effects of Ejecting From a Fighter Jet on the Spine
The need for speed places fighter pilots in electrifying yet dangerous situations. When things go wrong during flight, pilots must consider ejecting, a terrifying choice. Ejection is a last resort due to the large compressive forces and the high wind speeds that can cause many different serious injuries, including spinal injuries. Approximately 20-30% of people who survive ejection endure spinal fractures. Understanding the dangers of flight that service members face increases awareness of the military lifestyle within the civilian population and is critical in finding solutions to lessen the severity of injury.
Continue reading “Top Gun Trauma: the Effects of Ejecting From a Fighter Jet on the Spine”The Weight of Combat: Are powered exoskeletons the solution to heavy combat loads?
Have you ever wondered how much weight a soldier carries in a combat zone?
Continue reading “The Weight of Combat: Are powered exoskeletons the solution to heavy combat loads?”Why do bone fractures take a long time for healing?
Have you observed that someone around you has broken their arms or legs? Bone fracture is a complete or incomplete break of bone continuity. And it is very common in our daily lives that there are more than 3 million cases in the U.S. per year. Many events may cause bone fractures, such as falls, car accidents or sports injuries. So, do you know how long it takes for the fracture to heal?
Continue reading “Why do bone fractures take a long time for healing?”The Spinal Fusion that Reignited a Legendary Career
Can you imagine being the best player in the world at a certain sport and one day, aggravating an injury that not only put your athletic career in doubt, but also did not allow you to do normal daily activities? This is the challenge that faced Tiger Woods.
Continue reading “The Spinal Fusion that Reignited a Legendary Career”Skeletal Support Seekers’ Success (So Far)
Bones break, and broken bones need time to heal, or regrow. Fans of J.K. Rowling’s Harry Potter series are quite familiar with the concept of bone repair, as Harry is once required to drink a Skele-Gro potion to magically (and painfully) regrow his arm bones overnight. Now, as fantastic as it would be to completely fix broken bones in a few hours, modern medicine has not yet discovered that secret of the Wizarding World; however, several treatments have been developed in attempts to speed the rate of fracture repair as well as increase the comfort of the patient (take that, Skele-Gro).
Continue reading “Skeletal Support Seekers’ Success (So Far)”