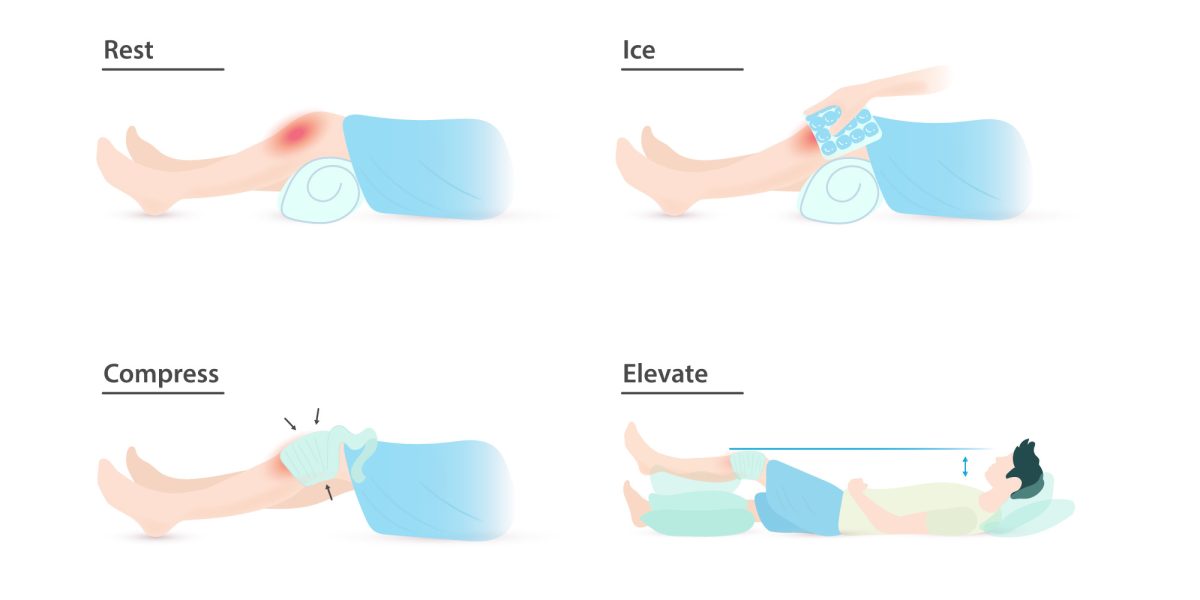
Have you ever been instructed to use the RICE protocol? Maybe you twisted your ankle on a root, slipped and fell hard on a patch of ice, or pulled your hamstring in an intramural soccer match. Rest, Ice, Compression, and Elevation is the common advice for immediate management of a soft tissue injury. But when you wrap a swollen calf, cover it with ice, and prop it on a pillow, what is actually going on beneath the skin? You may be able to feel the numbing cold of the ice and the compressive pressure of the wrap, but what about the healing processes that are harder to distinguish?
Continue reading “What are the RICE Method’s Impacts on the Healing Process Following Muscle Injuries?”Tag: treatment
Evolutionizing ALS Treatment: Can 3D-Printed Muscles Bring Hope to Patients?
ALS (Amyotrophic Lateral Sclerosis, a.k.a. Lou Gehrig’s disease) is is a rare but serious neurodegenerative condition that gradually causes muscle weakness and loss of control, eventually impacting the ability to move, speak, and breathe. It affects around 20,000-30,000 people in the U.S. at any time, with most cases diagnosed between ages 40 and 70.
Current ALS treatments are limited by a focus on symptom management and lack of understanding of the disease’s cause, but new technologies like 3D printing can offer exciting opportunities for innovation, such as custom prosthetics, artificial muscles, tissue engineering, and personalized medicine, which could significantly improve patient outcomes.
Continue ReadingUsing Vacuum Pressure to Heal Stroke & DVT Patients
Blocked blood vessels
Strokes are the 2nd leading cause of death worldwide. An estimated 795,000 people suffer a stroke every year in the United States. A stroke occurs when a blockage in a blood vessel leads to disruption or blockage of blood flow to the brain. Also, an estimated 350,000 people every year in the US suffer a deep vein thrombosis, which is when a blood clot forms in the deep veins often in the lower extremities. Venous clots can travel up the legs into the lungs or other vital organs, where they can become extremely dangerous or even fatal. When a blood vessel in a vital organ becomes occluded, blood flow must be restored as quickly as possible to return the patient to health.
There are two main procedural methods for removing blood clots from blocked arteries and veins: using tooling to extract the clot mechanically or using pressurized instruments to suck the clot mass out. Suction thrombectomies, also known as aspiration thrombectomies, are becoming more common because they have higher success rates of patient recovery.
READ MORETwists and Curves: Spinal Analysis and the Correction of Scoliosis
For anyone who had braces as a kid, you know how miserable the process can be. From rubber bands to the restrictions on what foods you could enjoy, having braces was a real pain. However, once the braces came off, it was all worth it to have perfectly straight teeth. While many adolescents go through orthodontic bracing to straighten crooked teeth, there are some who go through a similar process to correct the curvature of their spines.
Pressed and stressed: How understanding tumor biomechanics may be the future for treating patients with triple-negative breast cancer
Despite unstinting interventions such as chemotherapy and surgical tumor removal, approximately 40% of patients with stage I-III triple-negative breast cancer (TNBC) will experience tumor recurrence. Fortunately, not all hope is lost. The advent of immune checkpoint blockade (ICB) immunotherapy—a type of therapy that uses one’s own immune cells to kill the cancer—has shown great promise for the treatment of TNBC. However, as Dr. Azra Raza says in her book, The First Cell: And the Human Costs of Pursuing Cancer to the Last, these “immune approaches are not universally curative and, at present, help very few patients.”
Continue readingSensing tension in the brain tumor microenvironment
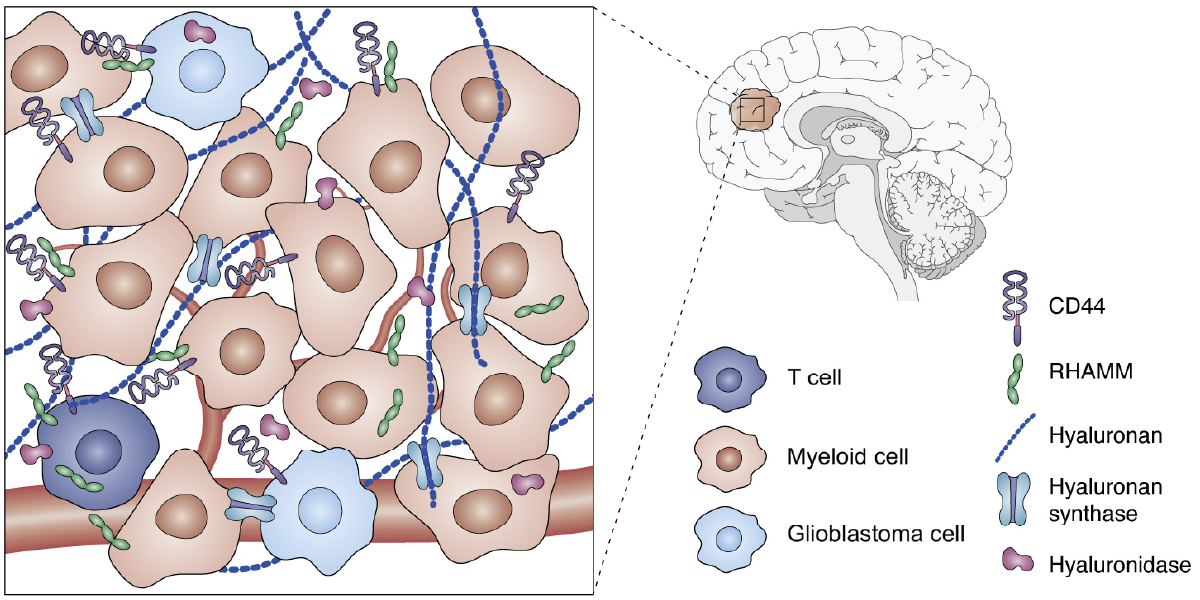
According to Azra Raza, a Professor of Medicine at Columbia University in New York, high-grade brain cancer called glioblastoma is “one of the most aggressive, ruthless killers known to mankind”. Indeed, despite recent advances in cancer therapies, glioblastoma remains incurable with a median survival of 15 months which has not improved substantially in the last 20 years. This poor prognosis is, in part, due to the highly immunosuppressive microenvironment that allows tumors to evade anti-tumor immune response and promotes resistance to immunotherapy – a kind of therapy that uses your body’s own immune system to find and eliminate tumor cells.
Continue reading “Sensing tension in the brain tumor microenvironment”Arthritis is NOT Just For The Elderly: Early Signs Of Rheumatoid Arthritis
Rheumatoid arthritis (RA) is a chronic autoimmune disease that, according to the Arthritis Foundation, affects 1.5 million people in the US. Women are 3 times more likely to develop RA and are usually diagnosed between ages 30 and 60, while men are rarely diagnosed before the age of 45.
Continue reading “Arthritis is NOT Just For The Elderly: Early Signs Of Rheumatoid Arthritis”What Can Different Types of Facial Wrinkles Tell Us?

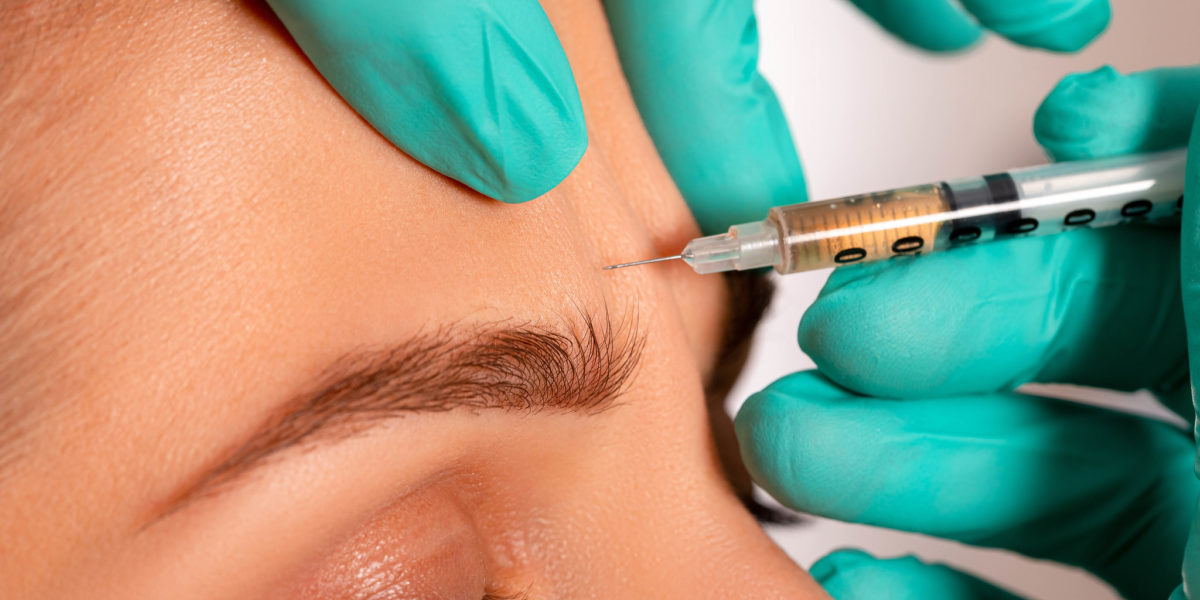
Few people enjoy having wrinkles. Some people spend a lot of time, money and efforts trying to reduce the wrinkles on their face, while others simply appreciate them as something naturally occurs with aging. Regardless, wrinkles are always associated with aging. However, if we look into what different types of wrinkles are and how they form, we will find that not all wrinkles are bad. Not all wrinkles are caused by aging, and not all wrinkles should be treated the same way. Here, we introduce different types of facial wrinkles categorized by plastic surgeon and their corresponding treatment.
Continue reading “What Can Different Types of Facial Wrinkles Tell Us?”Not Everyone Breathes While they Sleep: The Dangers of Sleep Apnea
You might think that breathing in our sleep should come naturally – if breathing and sleeping are both physiologically necessary, then we must be able to do them simultaneously right? Unfortunately, almost a quarter of middle-aged American men and nearly 10% of women suffer from sleep apnea, a chronic condition characterized by repeatedly stopping breathing while sleeping. The clinical symptoms seem rather benign – snoring, sleepiness, fatigue during the day or other issues sleeping. However, by far the most dangerous aspect of this disease is that it puts patients at increased risk of high blood pressure, stroke, coronary heart disease, as well as occupational and/or automobile accidents. Over the last several decades, a variety of therapy options have been studied to treat this condition, ranging from drugs to masks to surgery.
Continue reading “Not Everyone Breathes While they Sleep: The Dangers of Sleep Apnea”Ankle Sprains: An Epidemic in the World of Athletics
Have you ever been out running on a gorgeous fall day, only to have the run cut short by a painful misstep on a tree root covered by leaves? I have, and let me tell you – it’s awful! And even if you aren’t a runner, according to the Sports Medicine Research Manual, ankle sprains are a common, if not the most common, injury for sports involving lower body movements. Now, the solution to preventing this painful and annoying injury could be as simple as avoiding tree roots and uneven ground, but the real problem behind ankle sprains deals with the anatomy of the ankle.
Continue reading “Ankle Sprains: An Epidemic in the World of Athletics”